Dementia is a common and debilitating condition with enormous impact on individuals, families and communities. In 2015, 47 million people were estimated to be living with dementia globally. This number is projected to rise to 75 million by 2030 and 135 million by 2050.

The World Health Organisation (WHO) has declared Dementia prevention and treatment a public health priority.
Common symptoms include
- Memory loss
- Difficulty thinking
- Difficulty communicating
- Difficult with co-ordination and motor skills
- General confusion and agitation

Dementia can have a negative impact on your mental, physical and social wellbeing and many people consult their GP for advice on how to reduce their risk of developing this disease.
Most people ask what they can do themselves to reduce their risk of developing dementia.
We used to think that we are ‘stuck’ with the Genes we inherit form our parents but we now know that the situation is a little more complex than that.
Yes, we do inherit Genetic material from our parents but we now know that our environment has a big part to play in terms of if, when and how we develop conditions that had a genetic predisposition.
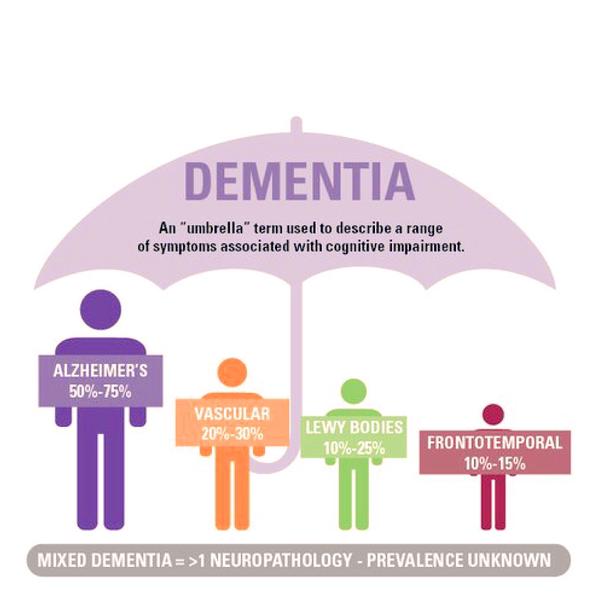
The most common form of Dementia is Alzhemier’s Disease (AD), which accounts for almost two thirds of all cases.
The remaining cases result form a number of conditions including parkinson’s disease, huntington’s choroea and vascular dementia.
We know that the pathological changes that occur in the brain in all of these conditions begin long before and clinical signs are apparent which gives us the opportunity to look for ways to intervene early in the disease process.
There have been many studies into possible prevention strategies.
Other studies have looked at what we can do to slow or halt the progression of mild cognitive impairment (MCI) to dementia. MCI is the presence of cognitive deficits ie impairment of function beyond what is expected for that age group but not severe enough to disrupt daily life. Each year about 10-15% of people with MCI progress to Dementia.
The World Alzheimer Report suggested that 48.4% of dementia cases can be attributed to modifiable lifestyle risk factors including:
- Smoking
- Midlife obesity
- Physical Inactivity
- Low Educational Attainment
- Diabetes
- Hypertension
- Major depressive disorder (MDD)
- Social Isolation or loneliness
Nutrition:
A recent review of 18 studies (5 of which were RCTs) showed that the Mediteranean Diet (diet based on fruits, vegetables, fish and olive oil) can help delay cognitive decline in several areas but they did not show any significant impact on the number of new cases of dementia. Dietry fibre intake of >30g per day has been shown to reduce your risk of dementia.
Other dietary interventions including diets high in omega 3 fatty acids, vitamin B complex, Vitamin E have failed to demonstrate any significant benefit. Some small isolated studies have been carried out to assess the benefits of green tea extract, concord grape juice, chromium picolinate, vitamin D and beta carotine but again, we don’t have enough evidence to support their use. There is some evidence to support the use of a diet low in saturated fat in combination with increased physical activity (Finnish Diabetes Prevention Study).
Weight:
Obesity can increase your risk of Type 2 Diabetes and high blood rpessure both of which icnrease your risk of developing both Alzheimer’s Disease and Vascular Dementia.
Physical Activity:
Evidence suggests exercise can both improve cognitive function in older adults with normal cognitive function as well as those with various levels of cognitive impairment.
It doesn’t seem to matter if the activity is aerobic or resistance based ie walking/tennis/golf versus weight training/yoga and the general consensus is that the amount of activity is more important than the type of activity. (Ladis, Rotterdam and Caerphilly Prospective studies). In these studies patients were physically active for between 90-180 minutes per week.
We think exercise reduces protects against the development and progression of dementia by increasing blood flow to the brain, by reducing inflammatory processes within the brain and by inducing producing protective factors in certain areas of the brain that protect our cognition.

Alcohol:
Alcohol excess has been shown to increase the risk of dementia.
High blood pressure, diabetes and high cholesterol
Multiple studies have shown that anti-hypertensives (medication for high blood pressure) may reduce the risk of cognitive decline vascular dementia and AD by 19-55 %.
The data for use of medication to reduce cholesterol (statins) has been less impressive and further studies are needed.
Association studies suggest that patients with diabetes have up to three times high risk of developing dementia. The risk is greater in women than in men. There does not seem to be much evidence to show reduction in progression of cognitive decline with treatment of diabetes.

Major Depressive Disorder (MDD):
MDD is strongly associated with increased risk for cognitive decline but we are unsure of the mechanism behind this and studies are ongoing into whether this in an inflammatory process or due to acummulation of certain proteins or other factors. In the meantime, we continue to focus on the treatment of MDD with medication, psychological support and lifestyle interventions.
Stress:
Psychological stressors have been found, in some small studies, to be associated with lower levels of cognitive performance and faster decline in brain function in both healthy adults and this with mild cognitive impairment.
There is some evidence from small studies to support the use of mindfulness based stressed reduction in those with cognitive impairment. Again, more research is needed.

Hope for the future:
There are ongoing studies looking at other lifestyle interventions such as intermittent fasting (IF), time restrictive feeding (TRF) and incorpotating diets rich in flavinoids (found in blueberries, wine and dark chocolate). Scientists are also looking into possible’vaccines’ to prevent dementia but lots more work is needed in this area.
In the meantime, if you are concerned about your risk of developing dementia go and see your GP.
