
This is a question which is increasingly being asked by people who I see in clinic, often because they have seen something about it on the TV or read about it in the news.
As things stand Type 1 diabetes can’t be cured. Management has however improved significantly over the last few decades. Gone are the days when you had to boil your needles and glass syringes in water, and measure your sugar by mixing urine, water and a clinitest tablet. Lots of people will still remember that. Technological advancements have produced blood glucose monitors that can be used at home, and now monitors that scan a device on your arm, allowing you to avoid finger pricking for blood tests completely.
Insulin is given through pen devices and pumps. Systems that both measure sugar and deliver insulin without you having to be so involved in the hour by hour decision making are also in development, and are being used experimentally. All the hurdles that have to be gone through to make sure these systems are safe for public use means this process takes a very long time.

It’s also an exciting time in the world of Type 2 diabetes, with the publication of clinical trials showing that it is possible for Type 2 diabetes to be put into remission with relatively achievable dietary changes, in certain circumstances.
Remission is a medical term which means the signs and symptoms of a disease have disappeared – it may be temporary or it may be permanent. In the case of diabetes there has been debate about the definition of remission but the major clinical trials define it as an HbA1c of less than 48 mmol/mol (6.5%), off all diabetes medications. HbA1c is a blood test used to measure diabetes control.
We know from previous studies of weight loss surgery that weight loss of around 15 kg is associated with remission of diabetes in about 75% of people. 15 kg is about 2.5 stones. This degree of weight loss is thought to cause enough loss of fat from within the liver and pancreas to allow them to start working normally again.

DiRECT is a clinical trial which was published in the medical journal “the Lancet” on 5th December 2017. DiRECT stands for Diabetes Remission Clinical Trial. The trial was undertaken by Profs Mike Lean and Roy Taylor and their research groups.
49 GP practices took part from Scotland and north-east England. People taking part were aged between 20-65 years, had had their diabetes for less than 6 years, had a body mass index of 27 – 45 kg/m² ie. in the overweight to severely obese range) and were not on insulin. HbA1c had to be under 108 mmol/mol (12%) at the start of the trial.
306 people took part. 149 of whom were in the intensive treatment group.
The people who were chosen for the intensive weight management group had all their diabetes and blood pressure tablets stopped. Instead of normal food they ate a meal replacement product of around 850 calories a day for 3 months although they could extend this to 5 months if they wished. Afterwards normal food was reintroduced over several weeks. They were given support and education about how to maintain their weight loss.
They were asked to continue their normal activities but not to introduce new activity. After the start of food reintroduction they were given step counters and encouraged to do up to 15 000 steps a day.
The people in the other group had normal care for their diabetes.
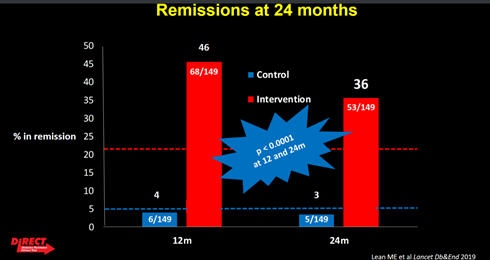
At 12 months almost half of the intensive treatment group (46%) were in remission from their diabetes. This compared to 4% of the other group. At 2 years 36% were still in remission.
The proportion of people who went into remission increased the more weight that was lost. 73% of those who had lost 10 kg went into remission, whereas in the group who had lost more than 15 kg (about a quarter of those in the intensive treatment group) 86% were in remission.
Quality of life was measured using questionnaires and had improved at 12 months in the intensive treatment group. No one had to withdraw from the study due to side effects, however 21% withdrew from before the end of the study for other reasons, the most common being “social reasons.”
There are a few caveats to think about with the trial. It is limited to patients with relatively recently diagnosed diabetes. There is evidence that weight loss on this scale is less likely to result in remission in people who have had Type 2 Diabetes for longer. The study was also performed in areas of the UK with mainly white populations so we don’t know if it applies to other ethnic groups. There was a high rate of people dropping out which indicates how hard it was to stick to the program. It was however very promising showing that at least in the short term significant weight loss using a very low calorie diet can lead to the remission of diabetes, without significant side effects.

What about Low Carbohydrate Diets?
Low Carbohydrate Diets are also promising in terms of both managing Type 2 diabetes and also of increasing remission rates. There are lots of clinical trials underway at present but no clear longer term trials looking at remission rates have been published as yet.
Having said that there is absolutely no doubt that people with Type 2 diabetes can significantly improve their blood sugars and some can get their HbA1c into the remission range while following a low carbohydrate plan. If you educate yourself with regards to the amount of carbohydrate that you are eating and make an effort to reduce it you are also highly likely to lose weight.

What if I put weight on and my Diabetes comes back?
We all know that losing weight on a diet is easier than maintaining weight loss afterwards, and that a lot of people do gradually put weight back over time. But we also know that even if you lose weight and your diabetes goes into remission for a couple of years and then comes back again – you will be in a better position by having had two diabetes free years in terms of your long term health, than if you hadn’t been in remission at all.
So times are very exciting and changes are happening in the way we, as doctors are thinking about Type 2 Diabetes. Access to programs like those in the DiRECT trial via the NHS is becoming easier in some parts of the country. There’s lots of freely available information available in relation to lowering carbohydrate intake in websites like Diabetes UK, along with meal plans etc. If you want to discuss these topics in more detail, the way diabetes services are set up varies from area to area but your GP of your Practice Nurse who deals with the people with Type 2 Diabetes in your GP Practice is likely to be a good starting point.

Importantly, if you have Type 2 diabetes and are on medication for it and you are considering making significant changes to your diet – discuss it with your medical team first, to ensure that medication doses are suitable.
Izzy