Mental Health is coming more to the forefront of National Health and Social Care Services as well as charitable foundations and rightly so.

It is estimated that 12.5% (roughly 1 in 8) of men in the UK are suffering from one of the common mental health disorders and this number is rising. (2) A pole of 1000 men carried out by the Priory in 2017 found that 77% of men had suffered with anxiety/depression/stress at some point in their lives.
Despite this, 40% of men won’t talk to anyone about their mental health, even their closest friends.
When asked who they would talk to, 66% said that they would share their feelings with their partner above anyone else. A worrying statistic in itself but very worrying for those who do not have a partner, or any close family or friend to confide in.
Some of the reasons men reported for not seeking help include:
- ‘I’ve learned to deal with it’
- ‘I don’t want to be a burden to anyone’
- ‘i’m too embarrassed’
- ‘There’s negative stigma around this type of thing’
- ‘I don’t want to admit I need support’
- ‘I have no-one to talk to’
In a 1 year period in Scotland there were 72 450 GP or practice nurse contacts made by men for anxiety and 54 990 for depression. Of these contacts the biggest number were seen in the 25-54 age group. (2)
A study carried out by the Royal College of Psychiatry in 2016 revealed that and 57% of men with depression were parents.
Again, the suspicion is that there is under reporting of symptoms on men surveyed. This hypothesis is backed by the following statistics:
- Men do report significantly lower life satisfaction that women in the Governments national wellbeing survey, with those aged 45-59 reporting the lowest levels of life satisfaction.
- 87% of rough sleepers are men (ref crisis)
- Men make up 95% of the prison population (ref House of Commons library) and 72% of male prisoners suffer from two or more mental disorders.
- Importantly, men have measurably lower access to the social support of friends, relatives and community. (Boreham and Pevali )
- Men are stressed. In a surgery of 1112 men conducted by Opinion Leader for the Men’s Health Forum 9% of employed males described themselves as feeling severely or extremely stressed.
- in the same survey, 34% said they would feel embarrassed of ashamed to take time off work for mental health concerns compared to 13% for physical injury.
Of the 5821 deaths from suicide in 2017, 75% were male with suicide being the leading cause of death in men under 50 years of age.
This amounts to 13 men taking their own lives each day, an entire rugby or football team.

Suicide is commonest among men who are separated, widowed or divorced.
It is more likely if you drink heavily.
There is a big overlap between anxiety and depression with many men presenting with a mixed picture of both of these conditions.
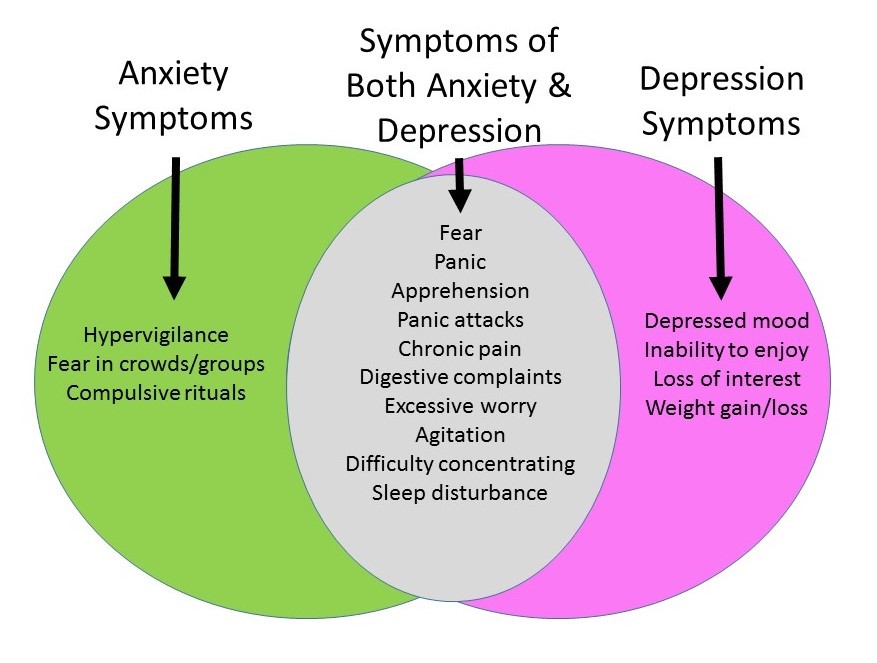
The Scottish Health Survey data indicates that among adults 11% report two or more symptoms of depression and 11% report 2 or more symptoms of anxiety, with women reporting more anxiety than men.
The term ‘anxiety’ refers to a broad category of conditions including social anxiety and generalised anxiety disorder.
Men may present with different symptoms of anxiety and depression than women and, as a result the diagnosis is often missed.
Symptoms that are more common in men include
- irritability
- sudden anger
- increased loss of control
- greater risk taking
- aggression
Their ways of coping may also be different. Men are diagnosed with anxiety and depression less often than women but their rates of heavy or dependent alcohol consumption and illegal drug use are greater than in women. In fact, 8.7 % of men are alcohol dependent compared to 3.3% of women. Similarly, 4.2% of men report frequent drug use compared to 3.3% of women.
It may be that instead of talking, men are using drugs and alcohol as ‘self medication’ to cope with their symptoms.

Common factors seen in depression and anxiety in men include relationship difficulties (the single thing most likely to make men depressed), major life events such as having children and the changes that brings to a relationship, work stress, financial problems or unemployment, alcohol excess, poor diet/lack of exercise and retirement with loss of daily structure.
Should you go and see your GP?

Men should be encouraged to speak to their GP if they feel they have symptoms of anxiety or depression. As a GP myself I would really hope that all my patients, men included would feel comfortable talking to me about their mental health, but the sad reality is that this is not the case.
There are many reasons for this. One of the big barriers is actually getting an appointment in the first place. GP practices, mine included, often use admin staff to ‘triage’ requests for appointments.
By this I mean they will ask you for a rough idea of what the appointment is for. While this information is really helpful for us in trying to get you an appointment with the right person, be in a P or nurse practitioner etc I am well aware it is another barrier to men, and women, actually getting in that chair in front of me.
Please be assured that a simple ‘It’s personal’ will suffice. We get this response several times a day. I would also suggest making a telephone consultation if this is either easier to get quickly or if you think you would be more comfortable speaking on the phone initially rather than face to face.
Also, if you are feeling really down, depressed or having thoughts about harming yourself or taking your own life, then ask for an emergency appointment. This is what these appointments are for and why we have them at the end of all of our surgeries. Again, if you don’t want to say what it is just say ‘it’s personal’.
The questions I ask someone when they come to see me with stress, anxiety or depression vary to some extent depending on the individual and on how much information they are happy to share with me. Sometimes, men just come in and say ‘I just don’t feel myself’ or ‘I just don feel happy’. Often they say their wife/girlfriend/mum has either encouraged them to make the appointment or has made it for them.
Sometimes, there isn’t much more information shared than that. This is also ok. It may be the firs time that person has met me or even been inside a GP surgery in years so I can totally see why they wouldn’t feel at ease letting a stranger know all their most personal thoughts.
I can still help you with this information. There are lots of things you can do to improve your mental health and loads of places to go for support.
More often than not, we take the time to gather as much information as we can to help us to come up with a plan of action together. The ten minute GP appointment goes out of the window here. If you need much longer than this, then that’s just fine and is often why us GP’s are running late.
If, based on information gathered above, we think medication would be helpful then we can usually get start right away. Equally, we can revisit this after giving you some information to take away and read.
There are also lots of other things we can suggest you look at in terms of your lifestyle that can have significant impact on your mental health.

Other things that may help alongside this include:
- Talking to someone-don’t bottle things up.?? Try to speak to a friend or family member about how you are feeling. If you are unable to talk about how you are feeling, write down your thoughts on paper.
- Eat well-anxiety and depression can have a negative effect on your appetite and people with these conditions often do not feel hungry. It is important to try to eat on a regular basis and aim for a balanced diet with lots of fresh vegetables and fibre and try to avoid too many sugary snacks.
- Avoid alcohol ??and drugs-often this is seen as a quick ‘pick me up’ but alcohol and drug use will increase symptoms of anxiety and depression, especially amphetamines and cocaine.
- Keep active-aim to be active every day, even if it’s just for ten minutes. ??♂️??♂️??♂️If possible be active outdoors but going to the gym is also a great idea. Activity reduces stress, increases ‘happy’ hormones including serotonin in your brains and aids sleep.
- Work on getting good quality sleep-sleep disturbance is very common in anxiety and depression. Try not to get too irritated on nights when sleep evades you but instead do something restful, try practising some mindfulness techniques (try the Headspace or CALM app for example) and avoid screen time before bed.
- Do something you enjoy-prioritise time in the week when you can do something you enjoy.⛳️??
- Reassess your goals-maybe you are expecting too much from yourself. Set realistic targets and make small changes to get you on the right path to beating your depression or anxiety.
- Read about depression-this may help you understand why you feel the way you do a little more.
- Consider trying yoga or meditation. Often overlooked as not seen as particularly ‘manly’ but there is a wealth of research to support their use in treating depression and anxiety and millions of men are using both yoga and meditation daily as part of their self care for their mental health. Just because yoga classes at the gym aren’t full of men, doesn’t mean men aren’t doing these things in the comfort of their own homes. I found both yoga and meditation intimidating concepts at first but I am seeing the benefits of adding small amounts of both into my day to day routine.
There are lots of places you can go for help and support via your GP or by self referral.
Many organisations, including Mind.org.uk, have useful guides on anxiety and depression.

Nationwide support groups include
- The Samaritans call 116 123 or use text service on 07725909090. Open 365 days
- Breathing Space call 0800 83 85 87. Open 365 days
- NHS 24 call 08454 24 24 24 open when GP practices closed
- CALM (campaign against living miserably) Calm Zone Helpline call 0800 58 58 58 open 5 to mid night 365 days
- Mind.org.uk call 0300 133 3393 text 86463 mon to fri 9am to 6pm
- No Panic (www.no panic.org.uk). Call 0844 967 4848
- Scottish Association for Mental Health SAMH.org.uk
- Andy’s man club

Some services available in Scotland and, more specifically in my local area of East Dunbartonshire include:
- East Dunbartonshire Association for Mental Health (www.EDAMH.org.uk)
- Brothers in Arms Scotland (www.brothersinarmsscotland.co.uk) Free to come along. Runs Thursday nights from 7pm in their unit in Stepps. They also now have a free to download app
- Brothers feel stress free APP-free to download
- The Changing Room at Tynecastle. Set up by Hearts Football Club to address men’s mental health
- See Me Scotland (www.seemescotland.org) funded by Scottish Government and Comic relief and run by SAMH has lots of support in local areas.
- Gary Faulds, local comedian runs a free met up support group for men with anxiety. Meetings are on Saturdays from 1.30 pm at Barmulloch Community Centre Glasgow
- The Men’s Shed community programme. Funded by Health Improvement Scotland (mensshed.org.uk) various sites with my local 2 being at St George’s Park Bearsden and Kilsyth Road Workspace Kirkintilloch.
Referrences
1.WHO world health report 2001
2. Men’s health forum 2017
3. ScotPHO Scottish Public Health Observatory