
Ischaemic heart disease was the number one overall cause of death in Scotland in 2017. It was documented as the cause of death in over 4000 men and around 2700 women. No one really knows why it affects more men than women.
What is it?
Ischaemic heart disease happens when there is hardening of the coronary arteries, the blood vessels which carry oxygen rich blood from the lungs to the heart. Some people can get a build up of a fatty substance called “plaque” in their arteries. The plaque hardens over time and partly blocks the blood vessel. This can happen to any of the arteries in the body but if it happens to the coronary arteries, it can mean that not enough oxygen rich blood can get to the heart.
If you have a plaque in your coronary arteries it may be that that enough oxygen gets to the heart while you’re sitting down resting, but when your heart needs more, for example when you are climbing up the stairs, the narrowing in the artery means not enough blood can get through. This can cause chest pain or discomfort, also known as angina.
Sometimes the surface of the plaque can burst. If this happens the contents of the plaque can cause a blood clot to form in the coronary artery which can potentially block the artery completely. The blockage can stop parts of the heart from receiving oxygen to the extent that areas of heart tissue are damaged beyond repair. This is commonly known as a heart attack. If enough of the heart is damaged it may lead to heart failure, abnormalities of the heart rhythm and/or death.

People that have early hardening of the coronary arteries may have no symptoms at all. As it progresses they may develop angina. Angina feels different to different people but classically it’s described as a pressure or pain across the chest, which may spread to the jaw or left arm. It tends to come on during activity eg. Walking up the stairs or up a hill. It usually goes away if people stop doing what they are doing.
If you have had any chest discomfort that isn’t easily explainable you should see a doctor so they can try and work out what’s causing it. It can be hard even for a doctor to tell from the description if symptoms are coming from the heart or if it could be something else, for example, indigestion and often you will need further investigations. If there is a suspicion it is heart related most hospitals have a chest pain clinic where you can be seen and assessed quickly, to see if further treatment or investigation is required.
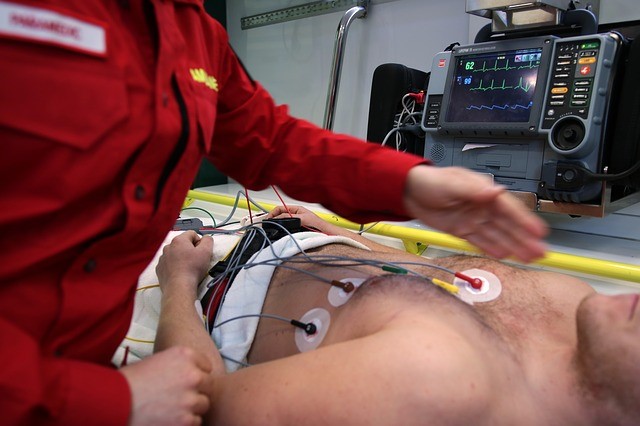
Importantly if your pain is severe, if it doesn’t go away quickly when you rest, or happens when you are not doing anything they you require urgent medical assessment in case you have had a heart attack. The chest pain that occurs in a heart attack is often in the same area as the chest pain in an angina attack, however it is usually more significant. It can be associated with sweating, shortness of breath, nausea and vomiting and palpitations (a sensation of an irregularity of the heart beat).
There are a number of tests that can be done to assess your heart, and it partly depends on the severity of symptoms. A heart tracing (ECG) can show up angina or a heart attack, but can be normal in between episodes of angina.
ECG stress testing is commonly performed for suspected angina. You walk on a tread-mill at a gradually increasing incline and speed. Before the test ECG leads are attached to the chest wall. If hardening of the coronary arteries is preventing enough blood getting to the heart during exercise, changes can often be seen on the ECG tracing. For people that aren’t mobile enough to walk on a treadmill, and in certain other circumstances various other tests can be done.

If test results show potentially significant coronary artery disease or if you have had a heart attack a coronary angiogram may be arranged. A thin tube is passed though one of the blood vessels in the wrist or the groin and into the coronary arteries. X-rays are used to make sure the tube is in the right place. Once it is in place, a special dye is injected which high-lights the coronary arteries. This allows areas of narrowing to be seen.
If there are areas of significant narrowing a tiny balloon can be inserted into the narrowing and blown up to widen the artery, or a tiny tube called a stent can be put into the narrowing to keep it open. Occasionally if there is widespread disease you may be referred to a heart surgeon for a bypass. Veins are taken from one of the legs or from the chest and attached to the coronary arteries in a way that bypasses the diseased area.
It some circumstances it can be appropriate to use tablet treatment to open up the blood vessels.
Who is at risk of ischemic heart disease?
-People with high “bad” cholesterol levels (LDL), and low “good” cholesterol (HDL)
-People with high blood pressure

-People who smoke as smoking can damage blood vessels, cause high blood pressure and raise cholesterol
-People who have pre-diabetes or diabetes
-People who are overweight or obese
-People who are not physically active as low activity levels can lead to unhealthy cholesterol levels, high blood pressure, being overweight or obese

-People who eat diets high in saturated fats and trans-fats, salt and sugar
-The older someone is, the greater their risk
-People with a family history of this kind of heart disease
People with sleep apnoea as it increases risk of high blood pressure and diabetes, and as well as increasing risk of heart attack and stroke in itself
People who are suffering from stress
People who drink too much alcohol
It’s clear from the list that although there are there are things we can’t do anything about like getting older and the illnesses that run in our family, the vast majority of risk factors are things that are within our control to change.
Many of the risk factors are inter-linked – making one improvement like improving your diet can impact on your weight, thereby reducing your risk of heart disease, but also of diabetes, sleep apnoea and high blood pressure. It can also have a direct impact on your cholesterol levels.

We know that if we do make healthy changes our risk of developing heart disease reduces. If a person already has a diagnosis of ischaemic heart disease making changes won’t reverse the damage but will prevent it from progressing. It’s never too late.
Izzy